What They Didn’t Teach You at University
Many professionals assume that if a patient is gaining strength, the muscle is “working properly.”
And if the patient sweats, shakes, or says they feel it… we assume the stimulus is adequate.
But the relationship between strength and muscle activity is far more complex.
When a muscle produces force, it also generates electrical activity. That activity can be measured through electromyography (EMG). However:
More force does not always mean more muscle activity. And more muscle activity does not always mean better results.
In this article, you will understand:
- – How strength and EMG are truly related.
- – When a muscle works… but does not actually get stronger.
- – How to avoid common mistakes in your treatments and strength programs.
Let me ask you something important:
How many of your patients do you think are “getting stronger”… when in reality they’re not reaching the necessary neuromuscular stimulus?
If you want to start making decisions based on objective data and eliminate unnecessary weeks of treatment…
1. Neural Adaptation Comes Before Structural Adaptation
The first thing you need to know is that during the first 4–6 weeks of training or rehabilitation, strength gains are not mainly due to hypertrophy.
They are due to neuromuscular adaptations.
The nervous system learns to:
- – Activate a greater number of motor units.
- – Increase the firing frequency of those units.
- – Improve synchronization between them.
- – Coordinate agonists and antagonists more efficiently.
- – Reduce unnecessary co-contractions.
This explains why a patient can gain strength without increasing muscle size.
From a clinical perspective, this is critical:
If you don’t generate sufficient neuromuscular activation, there will be no adaptation — even if the exercise “looks” correct.
2. Strength Gains Require a Minimum Level of Muscle Activation
EMG measures the intensity of the electrical signal the nervous system sends to the muscle.
For significant neural adaptation to occur, activation must exceed a certain threshold. In many clinical and performance contexts, it is considered that:
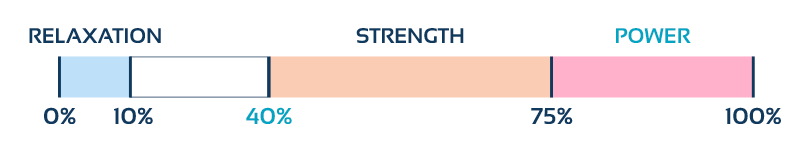
If activation does not exceed approximately 40% of Maximum Voluntary Contraction (MVC), the stimulus may be insufficient to generate meaningful strength gains.
What happens in practice?
Many exercises:
- – Are performed with loads that are too low.
- – Are executed with compensations.
- – Are performed in ranges where the target muscle is not the main contributor.
The result?
- – The patient works.
- – The patient feels effort.
- – But the muscle does not reach the necessary activation level.
And without sufficient activation, there is no relevant adaptation.
3. Feeling Effort Is Not the Same as Creating Adaptation
One of the most common clinical mistakes is confusing subjective perception with effective stimulus.
A patient may say:
“I really feel it.”
But that does not mean the muscle you intend to strengthen is the main contributor.
What may actually be happening:
- ❌ Another muscle is compensating.
- ❌ The effort is distributed across multiple structures.
- ❌ The target muscle is working below the adaptive threshold.
This is where measurement makes the difference.
When you use EMG, you can verify:
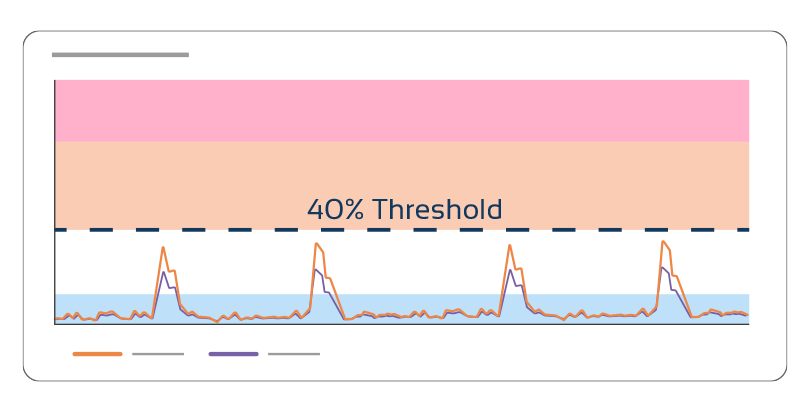
- ✅ Whether the target muscle is truly activating.
- ✅ Whether it reaches the required threshold.
- ✅ Whether asymmetries exist.
- ✅ Whether compensatory dominance is present.
Measurement eliminates guesswork.
4. Greater Activation Does Not Always Mean Greater Efficiency
According to Farina et al. (2014), a higher EMG signal may indicate greater neuromuscular effort. However, that increase in electrical activity is not always a positive sign. It can also reflect fatigue or even reduced neuromuscular efficiency.
A muscle may show higher activity because it is fatigued and needs to recruit more motor units to maintain the same force output. It may also be compensating for the weakness of another muscle, taking on a load that does not belong to it.
In these cases, a higher EMG signal is not a sign of improvement — but of overload or inefficiency.
In patients with pain, for example, elevated EMG activity may reflect protective overactivation or an altered motor pattern, not necessarily a favorable adaptation.
More activity does not always mean better performance or clinical progress.
That’s why EMG should never be interpreted in isolation. It must always be analyzed within the clinical context:
- The type of exercise being performed
- The load used
- The phase of rehabilitation
- The patient’s symptoms
- The therapeutic goal
Only by integrating all these factors can you give real meaning to the data and make precise decisions.
5. When a Muscle Works… But Does Not Get Stronger
A muscle can be active without truly getting stronger when the necessary conditions for adaptation are not met.
This can happen when:
- – It does not reach the minimum activation threshold, meaning the nervous system does not receive enough stimulus to improve force production.
- – It works intermittently or inconsistently, without maintaining sufficient intensity for long enough.
- – A stronger synergist dominates the movement, taking over most of the work and leaving the target muscle under-stimulated.
- – The movement occurs within an inefficient motor pattern, where coordination does not favor activation of the muscle you want to strengthen.
- – The external load is insufficient to recruit enough motor units to provoke adaptation.
- – Fatigue appears before the stimulus becomes effective, reducing repetition quality and limiting training impact.
In all these scenarios, treatment becomes unnecessarily prolonged — not because the patient isn’t working, but because the stimulus is not adequate to create change.
6. How to Apply This in Your Practice Starting Today
If you want to apply this knowledge practically:
- – Clearly define which muscle you want to strengthen.
- – Choose a functional and specific exercise.
- – Assess whether that muscle actually surpasses the activation threshold.
- – Adjust the load if it doesn’t.
- – Monitor compensations.
- – Reassess progress every few weeks.
The difference between a slow treatment and an efficient one often lies here:
It’s not how much the patient works.
It’s how and how much the correct muscle activates.
7. What EMG Adds to the Strength–Activation Relationship
With EMG, you can determine:
- ✅ Which muscle is actually activating.
- ✅ How much it activates (relative intensity).
- ✅ Whether it surpasses the adaptive threshold.
- ✅ Whether relevant asymmetries exist.
- ✅ Whether the exercise produces a neuromuscular response aligned with your goal.
You stop working on intuition, and start working with data.
Conclusion
The relationship between strength and muscle activity is neither linear nor automatic.
- – More strength does not always mean more activation.
- – More activation does not always mean efficiency.
- – Feeling effort does not guarantee adaptation.
If you don’t understand this relationship, you may be prescribing insufficient loads, reinforcing compensations, or unnecessarily prolonging recovery timelines.
The key is not doing more exercises.
The key is ensuring that the right muscle reaches the stimulus required to adapt.
Because in rehabilitation and performance, the winner is not the one who works the hardest, but the one who stimulates the nervous system most effectively.
Now let me ask you:
Are you sure the exercises you prescribe are generating the activation necessary for your patient to truly gain strength?
If you want to stop relying on sensations, better adjust loads, avoid invisible compensations, and accelerate recovery without guesswork…